What a Wound Care Clinic Does When a Leg or Foot Wound Won’t Heal

Maybe there’s a sore on your ankle that has been hanging around since January. Or a blister on the bottom of your foot that should have closed up two weeks ago, except now it’s bigger than when you first noticed it. Or some patch of skin near the shin that keeps weeping through whatever bandage you put on it. These are the wounds that creep into being problems without ever announcing themselves, and spring is when a lot of them surface. It’s the season when people stop layering up and actually look at what their lower legs have been doing all winter.
A healthy circulatory system closes most cuts and scrapes on its own within a couple of weeks. That’s what it’s supposed to do, in the background, with no input from you. So when a wound below the knee stops closing the way it should, the wound itself usually isn’t really the problem. Whatever’s holding it open is sitting deeper than that. Often in the blood vessels feeding the area. And treating the surface with drugstore supplies week after week mostly buys time you’d rather not be giving away.
A wound care clinic exists for that exact gap, where ordinary care has run out of road and something more targeted is what’s actually called for. Worth walking through what that more targeted care involves, because once the underlying cause gets addressed alongside the wound itself, the situation tends to look very different from where it started.
Why a Stubborn Wound Belongs at a Wound Care Clinic Instead of Under Another Bandage
When a wound hasn’t made meaningful progress in three or four weeks, it isn’t healing properly. Not by any reasonable definition of the word. That timeline isn’t arbitrary either. It’s roughly the window the body would normally use to close the gap if everything were working the way it’s supposed to. Once you’ve passed it, something is in the way of healing, and treating the wound the same way you’d treat a fresh scrape almost never changes the outcome.
The interference rarely comes from just one place. More often it’s a combination. Poor arterial flow starves the wound area of the oxygen and nutrients tissue needs to rebuild. Venous backup leaves fluid pooling under the skin and quietly breaking it down from below. Diabetes blunts nerve sensation, which means a small injury can go unnoticed long enough to deepen, and at the same time it slows the immune response that would otherwise hold an early infection in check. Most chronic wounds end up sitting at the intersection of two or three of these problems at once. That overlap is part of why something that looked uncomplicated at first ends up needing a more layered response.
Where a wound care clinic earns its place is in pulling the testing, the dressings, the procedures, and the vascular workup into the same building. The vascular piece matters more than it might sound. If circulation is the bottleneck, no amount of fresh dressings is going to close the wound until the blood flow itself gets sorted out. Treating the surface and ignoring the supply line is a setup for disappointment.
Signs You Need a Foot Ulcer Specialist and Should Not Keep Waiting
Foot wounds in particular have a way of pulling people into a cycle of adjusting the bandage and waiting things out. Some of them do turn around on their own. Plenty of others sit in place, or quietly get worse, and the warning signs that things have moved into ulcer territory aren’t always obvious enough to make you act on them.
The signs worth taking seriously:
- A sore on the foot or leg that has been there for more than three weeks without visibly shrinking
- Drainage that keeps soaking through dressings, particularly if the fluid has changed color or developed any kind of smell
- Skin around the wound that looks darker, harder, or more inflamed than it did a week ago
- Pain that wakes you at night, or that’s steadily getting worse instead of easing up
- Numbness around the wound, which is its own kind of warning because it usually means the nerves in the area have already been affected by something deeper down
- Any sore on the bottom of the foot in someone with diabetes, no matter how small it looks or how little it hurts
That last bullet comes with its own asterisk. Diabetic foot ulcers are often painless in the early stages because the nerve damage that goes along with diabetes blunts the warning system that would normally tell you something is wrong. A painless wound on a part of the foot you can’t easily see is exactly the kind of thing that gets ignored until it’s progressed somewhere serious. A foot ulcer specialist is trained to catch these well before they get there.
How Leg Ulcer Treatment Begins With Finding What Is Behind the Wound
Real leg ulcer treatment starts well before anyone actually touches the wound. The first job is figuring out what’s feeding the area, or in many cases what’s failing to feed it, because the cause shapes everything that comes after.
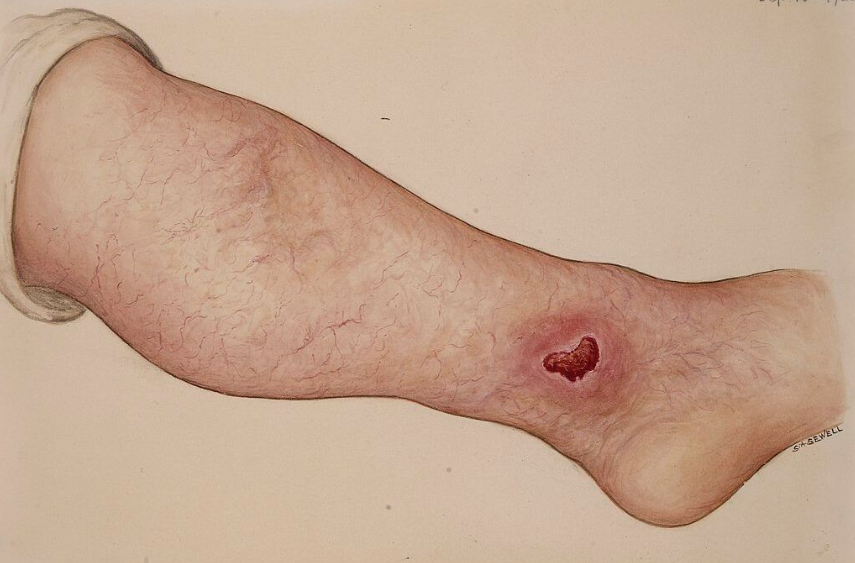
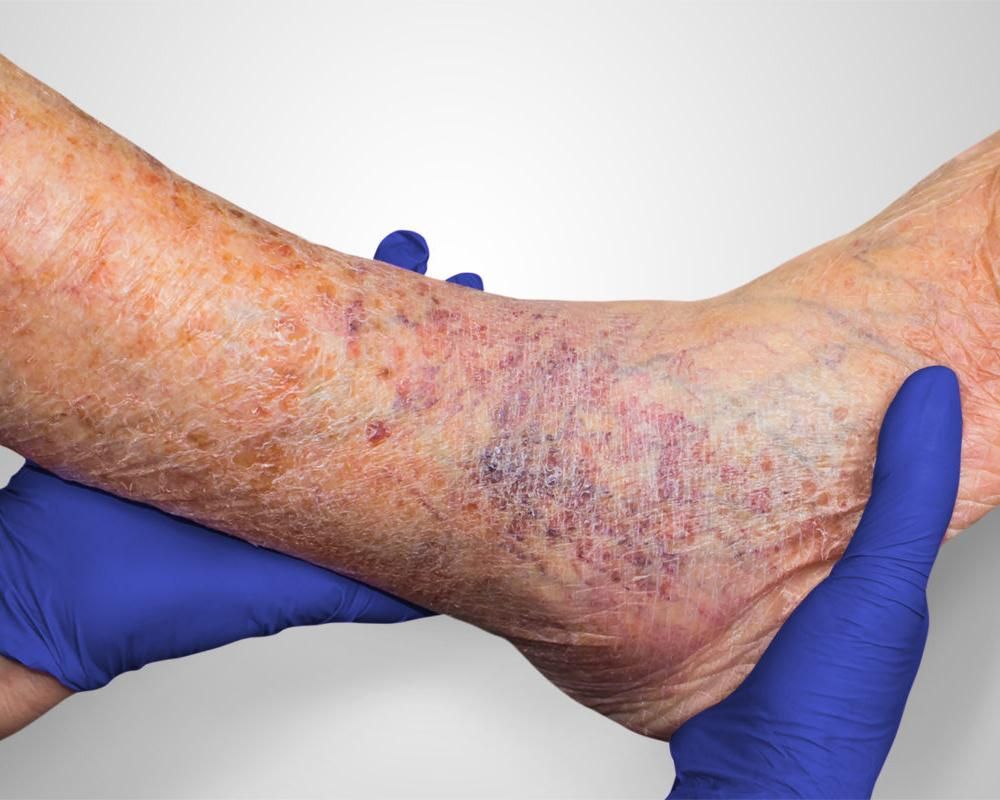
For most lower-leg ulcers the question is whether the problem is arterial, venous, or some mix of both. Arterial ulcers tend to show up on the toes, the outer ankle, or other pressure points, and they often look pale with dry edges that are sharply defined against the surrounding skin. Venous ulcers are more common just above the inner ankle, and they usually bring a brownish discoloration in the surrounding tissue from the chronic backup of blood. Diabetic neuropathic ulcers typically land on the bottom of the foot, under the ball or on the heel, wherever pressure builds up most during walking. Location alone gives a vascular specialist a strong starting hypothesis, but the imaging is what confirms it.
Duplex ultrasound shows the circulation in real time. It tells us whether arteries are narrowed, whether vein valves are leaking the wrong way, and where the trouble spots are concentrated. The ankle-brachial index, which is just a comparison of blood pressure at your ankle versus your arm, takes about fifteen minutes and gives a quick read on whether arterial flow to the lower leg is where it should be. When the picture needs more detail than that, CT angiography lays the arteries out in three dimensions. None of this is really about the wound on the surface. It’s about the system underneath that’s supposed to keep wounds from getting to this point in the first place.
What a Foot Ulcer Specialist Actually Does in the Treatment Room
Once the diagnosis is settled, treatment usually has to move on a few fronts at once. The wound itself needs care. The underlying cause needs to be dealt with. And anything that’s actively making the situation worse, whether that’s pressure on the spot, a low-grade infection, or swelling that won’t quit, has to come under control too.
Tools and Techniques Used in Leg Ulcer Treatment
Debridement usually comes early. Dead or damaged tissue at the edge or base of the wound has to come off before healthy tissue has any room to grow in and replace it. There are a few different ways to handle that, and the choice depends on what kind of wound you’re working with. Sharp debridement uses surgical instruments and is the most direct method. Other approaches lean on enzymatic dressings, controlled irrigation, or biological methods the body can handle over a longer time frame.
Specialty dressings are the next layer. Some are built to hold moisture in when the wound is too dry. Others pull fluid out when it’s weeping more than it should. And then there are biological dressings, which essentially act as a scaffold for new tissue to grow into. The right dressing isn’t a fixed answer. It depends on what the wound looks like that week, and it changes as the wound progresses, which is part of why these visits happen on a regular schedule rather than as a single appointment you book and forget.
Compression therapy does most of the heavy lifting on venous ulcers, alongside the dressings. Multilayer compression wraps bring down the swelling and back-pressure that have been keeping the wound open, and once they’re going on consistently the wound usually starts behaving differently. Wounds that are draining heavily or just refusing to make any progress sometimes call for negative pressure wound therapy, which uses gentle suction to draw fluid out and help pull the edges of the wound closer together. It looks more involved than it really is once you see how it actually works.
When Hyperbaric Oxygen Becomes Part of the Wound Care Clinic Plan
Some wounds need more oxygen than the bloodstream can deliver under ordinary conditions. Hyperbaric oxygen therapy is what answers that. It involves breathing oxygen through a delivery hood while you sit upright in a reclining chair, and the result is an oxygen concentration in your blood well above what you’d ever see at normal pressure. The extra oxygen helps damaged tissue rebuild, gives the immune system more to work with against lingering infection, and can move the needle on wounds that have been stuck in place for months at a time.
Not every wound is a candidate for it. Hyperbaric oxygen tends to be held in reserve for cases where standard approaches have plateaued, or where the underlying tissue damage is severe enough that the wound just can’t generate its own healing without outside help. When it is the right call, it’s one of the more effective tools available at a wound care clinic.
If circulation is the limiting factor, the conversation has to turn to revascularization at some point. Restoring blood flow through the artery feeding the area can take a wound that’s been stuck for months and put it back on a normal closing timeline. That’s part of why having a vascular specialist involved in your leg ulcer treatment makes a real difference. The vessels and the wound get treated as one problem, in the same place, by people who already understand how the two are connected.
What Recovery Looks Like Once Leg Ulcer Treatment Is Underway
Wound healing isn’t fast, and being honest about that up front matters. Week three won’t look dramatically different from week one, and going in expecting otherwise is a setup for frustration. Most chronic wounds take anywhere from weeks to months to fully close. The exact timeline depends on what caused the wound, how big it is, and how much underlying disease is in the picture alongside it. Progress tends to come in stages. First the wound stops getting worse. Then the edges start to pull in. Then new tissue fills the base. And finally the surface skin grows back over the top.
Visits typically run once or twice a week through the active treatment phase. Each one means assessing the wound, changing the dressings, adjusting compression, and deciding whether anything in the plan needs to shift. Between visits there’s a home care routine to follow, and how closely that gets followed has more impact on the timeline than it might sound like it should. Wounds that close fastest are usually the ones where the home portion is being treated as seriously as the clinic visits.
There’s one more piece worth mentioning, and it’s what happens after the wound finally closes. Skin that was once an ulcer is more fragile than the rest of your skin, and it stays that way for a long time after the visible healing is done. Maintenance matters here. Moisturizing the area, watching for early signs of breakdown, continuing with compression if that was part of the plan, and following through on whatever vascular condition contributed in the first place. Skipping any of those steps is the most common reason a healed wound becomes a recurring one.
Schedule a Visit With a Foot Ulcer Specialist at Our Hillsdale Wound Care Clinic
If you’re looking at a sore that should have closed by now, or a foot wound that keeps coming back to the same spot, the most useful thing you can do is get it evaluated by someone who works with these conditions regularly. At Advanced Veins and Vascular in Hillsdale, our wound care clinic serves patients from across Hillsdale County and Coldwater, along with Adrian, Jackson, Sturgis, and Toledo. Diagnostic testing, the vascular workup, and the treatment itself all happen under one roof, so you aren’t bouncing between offices trying to get a coherent answer.
Call (517) 836-3443 to book a consultation. A first visit gives you a clear picture of what’s keeping the wound open and a realistic plan for closing it, so you can stop changing dressings on something that hasn’t changed in weeks and watch the wound actually start to shrink instead.