How a PAD Specialist Finds and Treats Poor Leg Circulation Before It Gets Worse

It almost always starts the same way. You are crossing a parking lot or walking up a slight hill and cramping hits your calf. You stop. Wait maybe thirty seconds. The pain fades. You keep going and it comes right back, same spot, same intensity. You blame it on being out of shape or on age and move on with your day. Then it happens again tomorrow. Same leg. Same distance. Same cramping.
That pattern - predictable leg pain with activity that goes away when you rest - is one of the clearest signals of peripheral artery disease, or PAD. The arteries that feed blood to your leg muscles have narrowed to the point where supply cannot keep pace with demand once you start moving. A PAD specialist can find exactly where the narrowing is, figure out how far it has gone, and lay out what it takes to get you walking comfortably again. And the sooner that evaluation happens, the more treatment options remain on the table.
What a PAD Specialist Is Actually Looking For Inside Your Arteries
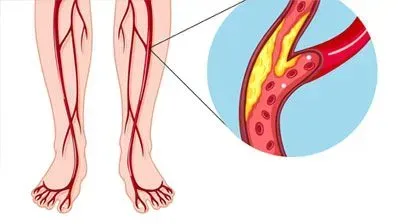
PAD comes down to plaque buildup. Fatty deposits collect along the inside walls of your arteries over the years and gradually narrow the channel blood flows through. Same process that causes heart attacks when it happens in the coronary arteries - except here it is happening in the arteries feeding your legs. While you are sitting or standing still, enough blood squeezes past the blockage to keep your muscles satisfied. Start walking and those muscles demand a lot more oxygen. The narrowed arteries cannot deliver it. That is the cramp.
Somewhere between 8 and 12 million Americans have PAD. Most of them do not know it. The symptoms creep in so slowly that people adjust around them without realizing what they are doing - parking closer to store entrances, taking fewer walks, sitting down more during the day. I have had patients come in and say they thought they just lost interest in walking. They had not lost interest. Their legs had been telling them something was wrong for months and they adapted instead of asking why.
And PAD is not only a leg problem. If plaque is accumulating in the arteries running through your legs, chances are very high it is building in your heart’s arteries and the vessels going to your brain as well. That is why people with PAD have a significantly higher risk of heart attack and stroke. Seeing a vascular doctor in Michigan about your leg pain is also about protecting the rest of your cardiovascular system, even if the legs are what brought you through the door.
Leg Pain Treatment Starts With Knowing What These Symptoms Mean
The medical name for that activity-triggered leg pain is intermittent claudication. Patients describe it differently. Some say cramping. Others call it a deep tightness or a heaviness that makes the leg feel like it weighs twice what it should. Where the pain shows up tells us something about where the blockage is. Calf pain usually means the narrowing is at or below the knee. When it hits the thigh or buttock area, the problem tends to sit higher up in the iliac or femoral arteries.
The thing that separates claudication from an ordinary muscle strain is how predictable it is. Patients can practically time it. One block of walking. Half an aisle at the grocery store in Coldwater. Fifty feet past the mailbox. That kind of consistency points squarely at an arterial problem, not a muscle or joint issue.
Beyond the cramping itself, a PAD specialist watches for quieter signs:
- Feet or toes that feel cold even in a warm house
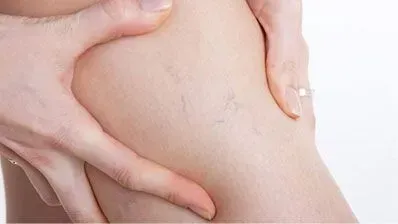
- Skin on the lower legs that looks shiny or unusually smooth. Hair growth that has slowed down or stopped altogether. A lot of patients do not connect those changes to circulation, but they are telling signs.
- Pulses in the feet that feel weak or absent when we check them during the exam
- Toenails growing slower than they used to
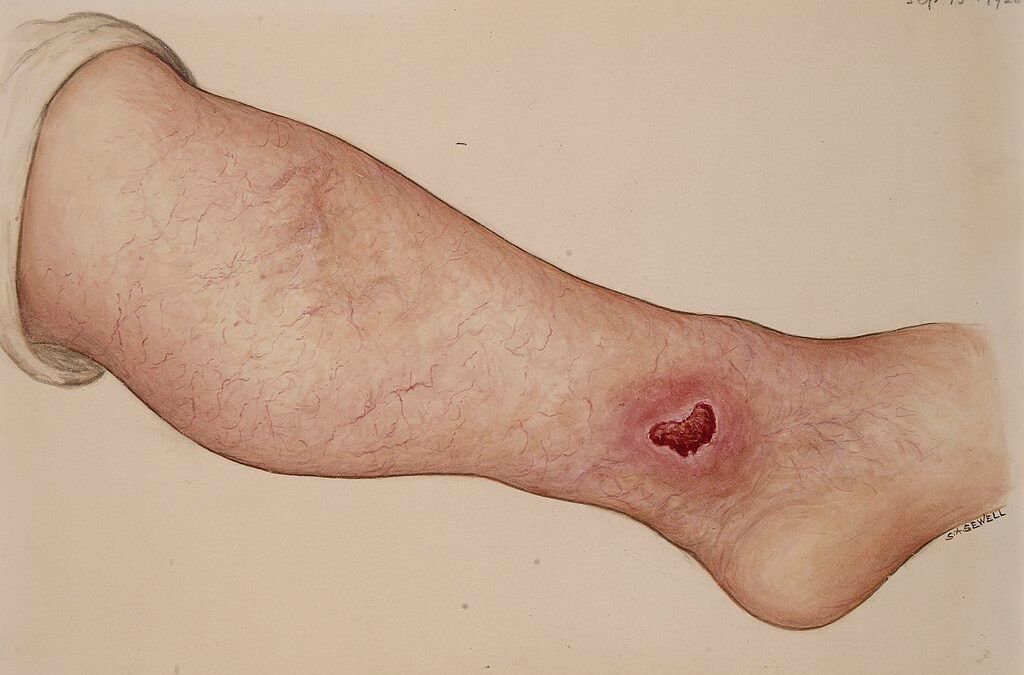
- Sores on the feet that take weeks to heal or do not close at all
- A noticeable pallor when you raise your legs above heart level
When leg pain starts deciding your schedule for you - no more walks, avoiding stairs, dreading the parking lot at Meijer - that is your signal to pursue leg pain treatment with a specialist who can determine whether your arteries are the cause.
How a Vascular Specialist Diagnoses PAD in Hillsdale County
The first test is disarmingly simple. We take a blood pressure reading at your ankle and another at your arm. Compare the two numbers. In a healthy system they land close together. When the ankle number drops well below the arm, blood is not getting to your lower legs the way it should. That test is called the ankle-brachial index, or ABI. Fifteen minutes, two blood pressure cuffs, and we already have a solid baseline answer.
But a number alone does not tell a vascular specialist where the problem sits or how extensive it is. For that we use duplex ultrasound - it shows the arteries in your legs in real time, lets us measure blood velocity, and pinpoints the exact spots where narrowing has developed. We can see the plaque and judge how much of the channel it is occupying. No needles, no radiation, no discomfort.
We sometimes have patients walk on a treadmill and then recheck the ABI immediately after. The idea is to recreate the conditions that trigger your symptoms and match what you feel with measurable changes in blood flow. It is one thing to say "my calf hurts when I walk." It is another to show that the ankle pressure drops 40 points after two minutes of walking. That kind of data tells us exactly what we are dealing with.
For patients who need imaging before a procedure, CT angiography provides detailed three-dimensional maps of the arteries. All of this testing happens at our Hillsdale office. No referral to another facility. We handle it here.
Vascular Claudication Treatment: What the Options Actually Look Like
Where we start depends on how far the disease has progressed and how much it is affecting your daily life. A PAD specialist puts together a plan that works on the problem from several directions at once.
Walking Programs That Work for Early PAD Leg Pain Treatment
This sounds counterintuitive, but bear with me. The protocol is to walk until the cramping starts, stop and rest until it fades, then walk again. Repeat that several times a week. Over the course of a few months your body responds by growing collateral blood vessels - small alternate pathways that route blood around the blockage. It is like your circulatory system building a detour. Patients who stick with structured walking for eight to twelve weeks are often genuinely surprised at how much farther they can go before the pain sets in.
And then there is smoking. If you smoke and you have PAD, quitting is the single most impactful thing you can do. I am not saying that lightly. Tobacco damages artery walls directly and accelerates plaque buildup faster than almost any other factor. I have watched patients’ walking distance improve after quitting, with no other changes to their treatment plan. Diet matters too - getting cholesterol and blood sugar under control slows the plaque from accumulating further. None of this is exciting advice, but it is the foundation that vascular claudication treatment is built on. Skip it and the rest becomes less effective.
Medications a PAD Specialist Uses to Manage the Disease
Most patients with PAD end up taking a few medications working on different fronts. Antiplatelet drugs like aspirin or clopidogrel make it harder for clots to form at the narrowed sections. Statins pull cholesterol numbers down and also stabilize the plaque already stuck to the artery walls, making it less likely to crack and cause a sudden blockage. Blood pressure medications protect the arteries from ongoing wear.
There is also a drug called cilostazol that specifically targets claudication symptoms. It can extend how far you walk before the pain kicks in. Not everyone can take it - if you have heart failure it is off the table - but when it works, patients notice.
Medication will not reverse blockages that are already there. What it does is slow the disease meaningfully and reduce the cardiovascular risk that comes alongside PAD. For patients with mild or moderate symptoms, walking programs plus medication is often enough to get them back to a quality of life they had written off.
Minimally Invasive Vascular Claudication Treatment When Conservative Approaches Are Not Enough
When lifestyle changes and medication cannot keep up with the disease, procedures that physically reopen the artery become the next step. These are done through a small puncture, usually at the groin, with catheters guided to the blockage by real-time imaging. You stay awake. Local anesthesia keeps things comfortable.
Angioplasty is the most common approach - a tiny balloon on the tip of a catheter gets inflated at the narrowed point, pressing the plaque against the artery wall and widening the channel. A stent, which is basically a small mesh scaffold, may be placed to hold things open afterward. Atherectomy takes a different route and shaves or removes plaque directly from inside the artery. Most patients go home the same day. Recovery is days, not weeks.
Bypass surgery is still an option for patients with blockages that are too long or too complex for a catheter-based fix. The vascular specialist uses either a healthy vein from elsewhere in your body or a synthetic graft to build a new channel for blood flow around the obstruction. Bigger procedure, longer recovery, but for certain patterns of disease it gives the most durable long-term result.
What Happens When You Put Off Leg Pain Treatment With a PAD Specialist
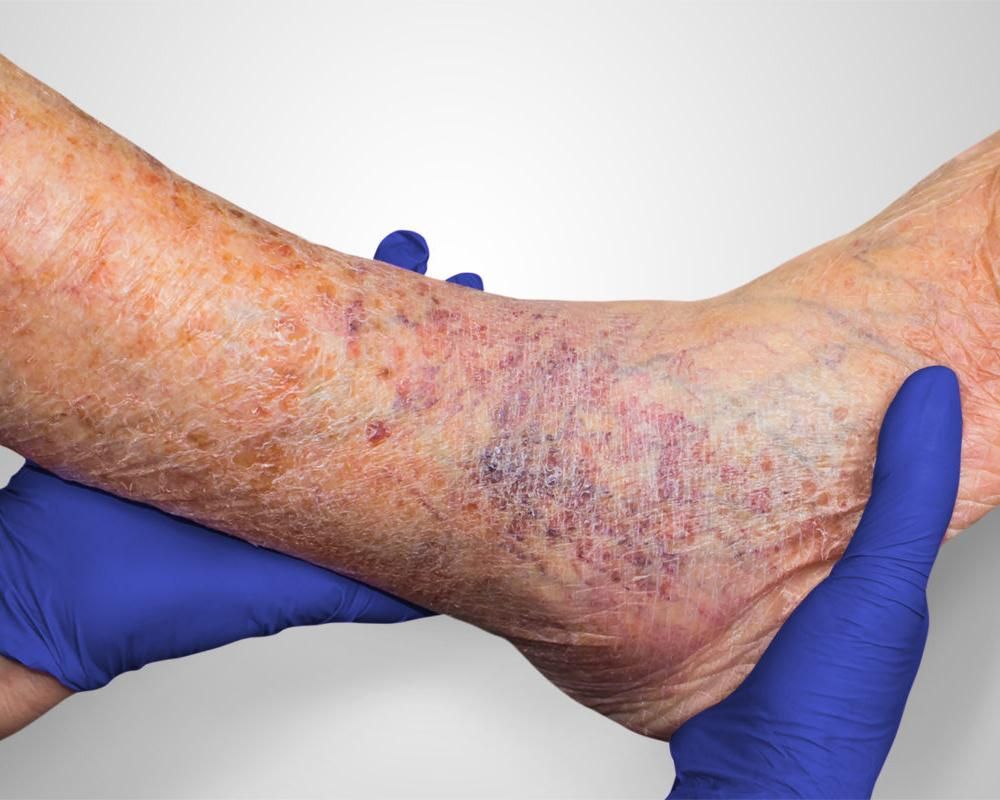
PAD does not hold still. Claudication that starts as a nuisance can progress to a condition called critical limb ischemia, where blood flow drops so low your tissues cannot get enough oxygen even when you are sitting in a chair. At that stage you are looking at rest pain, wounds on the feet that will not close, and a real risk of tissue loss and amputation. That is not meant as a scare tactic. It is what happens when this disease runs without intervention.
The slide from early claudication to critical limb ischemia takes months to years, not days. But every stage narrows what we can do to help. A patient who comes in with early symptoms might only need walking programs and medication tweaks. That same person, a couple years later with discolored toes and an open wound, may need emergency revascularization and months of wound care at our clinic. I have seen both versions of that story play out, and the contrast in what the patient goes through is hard to overstate.
Then there is the cardiovascular piece. People living with PAD face a higher incidence of heart attack and stroke than those without it. Working with a vascular doctor in Michigan who treats PAD as a systemic disease means that broader risk gets managed alongside the leg symptoms. Not one or the other. Both.
Schedule Your PAD Evaluation With a Vascular Specialist in Michigan
If walking has become something you plan around rather than something you just do, it is worth finding out why. At Advanced Veins and Vascular in Hillsdale we provide full PAD evaluation and vascular claudication treatment for patients across Hillsdale County, Coldwater, Adrian, Jackson, and Sturgis. Diagnostic testing, treatment planning, and procedures all happen here. One location.
Call (517) 948-0966 to schedule your consultation. A 15-minute screening test tells us whether your leg pain is an artery problem, and from there we put together a plan to get you back to covering ground without stopping every hundred yards to let the cramping pass.